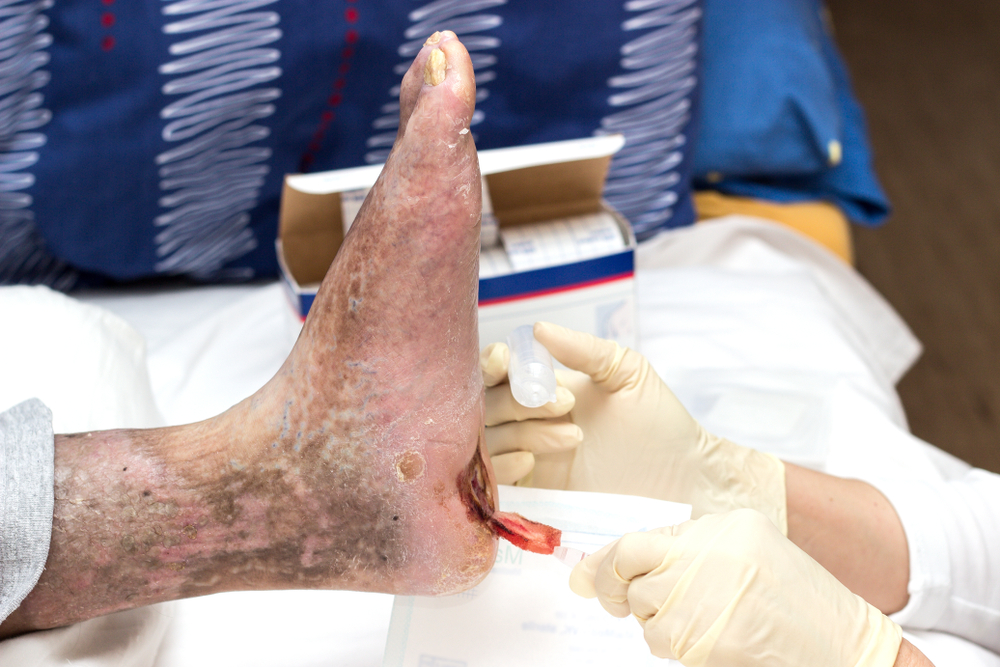
The main risk factors for Patients with Diabetes are peripheral neuropathy, peripheral arterial disease and structural deformity.
Peripheral neuropathy is when you have altered sensation or numbness in the feet and/or hands which can lead to ulceration, oedema (swelling) and if left untreated, sepsis, osteomyelitis, and amputation. Ulceration can often start as a simple callous, blister or embedded foreign object such as a splinter. Due to the lack of sensitivity in the feet, these anomalies can go unnoticed until the skin breaks down.
Peripheral arterial disease is another common cause of foot ulceration. Cuts and abrasions or excessive pressure can lead to amor infections in patients with diabetes as they tend to have weaker immune systems. Left untreated infections can lead to gangrene and go right down to the bone, where the wound is unlikely to heal. Sepsis (blood poisoning) then becomes a major risk and amputation may be required. Smoking cessation is recommended for at-risk patients to reduce the risk of Peripheral arterial disease and associated complications.
Bone deformity and joint mobility problems can further contribute to the formation of ulcers and infection, due to increased pressure in prominent bony parts. Well fitting footwear, socks and the use of pressure-deflecting insoles or orthoses are vitally important to prevent pressure problems from arising. Mobilisation of foot joints and a good exercise regime for the feet is also important.
Patients with a High-Risk foot should have their feet examined by a Podiatrist at least once a year to assess and monitor the risk. This exam will assess protective sensation, foot structure and biomechanics, vascular status and skin integrity. Appropriate advice and education will also be given. Good foot care will halve the risk of disease related amputation.
